The IoP Complex is the physical and institutional home of Preemptology — a purpose-built ecosystem in which training, clinical care, and the generation of evidence operate not in isolation, but in continuous, deliberate relationship.
Structured around three interconnected pillars, the Complex trains a new generation of physician-leaders, provides specialist and community-level care, and demonstrates — measurably — that the burden of preventable early death can be systematically reduced. It is a founding institution.

The IoP Model — Three Pillars, One Ecosystem

The Institute is the operational and intellectual core of the Complex. It trains and certifies Preemptologists — medical doctors equipped to lead population-scale preventive care — and coordinates their deployment across defined health zones.
At its centre is the Preemptorium, a specialist referral facility that receives complex cases escalated from the field. Alongside it, a network of City Consultants — senior specialists reoriented to community-facing roles — ensures that advanced clinical expertise reaches the people who need it most.
Explore the Formation Model →
The IoP Medical School is the first of its kind to embed Preemptology into the foundations of medical training. From the earliest years of study, students learn to think preemptively — not simply how to treat illness, but how to anticipate, detect, and organise against disease at a population level.
Graduates emerge as physician-leaders: clinically grounded, health-systems literate, and equipped to work at the intersection of medicine, public health, and institutional design. They are trained to reform health systems from within.
The Principles of Admission →
The Comprehensive Cancer Centre is not a supplementary wing of the Complex — it is its strategic anchor. Within the IoP's mandate for whole-person prevention, one disease leads: cervical cancer. Not because it is the most prevalent, but because it is the most instructive. The science is settled. The tools exist. A disease that is wholly preventable should not be claiming a thousand lives every day.
That it does reflects a failure of operational ownership — the kind of failure Preemptology is built to correct. Cervical Cancer Elimination is therefore the IoP's flagship programme: the first demonstration of what an operationally organised system of prevention can achieve, and the template for every disease-preemption effort that follows.
Where invasive cervical cancer does occur, it represents earlier opportunities that were missed. A Comprehensive Cancer Centre is the completion of prevention — ensuring every woman, wherever she sits along the disease continuum, receives the full spectrum of care the system owes her.
Cervical cancer can be eliminated as a public health threat. The WHO has defined the targets every country must reach by 2030 to set that process in motion. The IoP's flagship programme is built to operationalise them.
90% of girls fully vaccinated with the HPV vaccine by the age of 15, establishing population-level immunity before exposure.
70% of women screened using a high-performance test by age 35, and again by age 45, detecting disease before it advances.
90% of women with pre-cancer treated; 90% of those with invasive cancer fully managed. Treatment completes the continuum where earlier prevention was not reached.
Elimination is defined as a sustained incidence rate below 4 per 100,000 women. The Comprehensive Cancer Centre provides the clinical capacity necessary for the third pillar of this framework — without which elimination remains incomplete.
The IoP Complex will launch through a focused set of institutional pilots. Each will establish the Institute in a defined health zone, deploy the full referral and coordination structure, and track clear early indicators — including vaccination coverage, screening rates, early detection outcomes, and referral completion. The evidence gathered will shape the operational model for broader replication.
Establish the founding cohort of Preemptologists, rigorously trained and credentialled to lead the field.
Deploy the model across three defined health zones, generating the evidence base for institutional validation.
Translate pilot findings into a replicable operational framework for phased global expansion.
The IoP Complex will be built in Africa, and within Africa, in Enugu — a deliberate choice grounded in epidemiology, institutional readiness, and historical precedent.
To build a health system that works everywhere, you must first prove it works where the conditions are hardest. Africa offers precisely that challenge — and precisely that opportunity. Solutions developed in resource-constrained settings are forged for efficiency. A model that succeeds here carries a transferability that no high-income-context model can match. By beginning its work on the continent, the IoP builds not for Africa alone, but from Africa — developing approaches intrinsically suited for every comparable setting in the world.
Efficiency born of constraint is efficiency that travels. Operational models tested in low-resource environments are intrinsically suited for the comparable settings where the greatest burden of preventable disease persists.
Sub-Saharan Africa has the lowest density of healthcare workers of any region in the world. By training Preemptologists here, the IoP addresses this structural gap at its root — developing the human infrastructure where its absence is most consequential.
The continent faces a compounding challenge: persistent infectious disease alongside a rapidly escalating burden of non-communicable conditions. This dual crisis demands the integrated, preemptive, whole-person approach that Preemptologists are specifically trained to deliver.
Among the cities of the continent, Enugu stands apart. Its advantages align precisely with the A.C.I.D. framework — a practical test of institutional readiness for the IoP's founding operations.
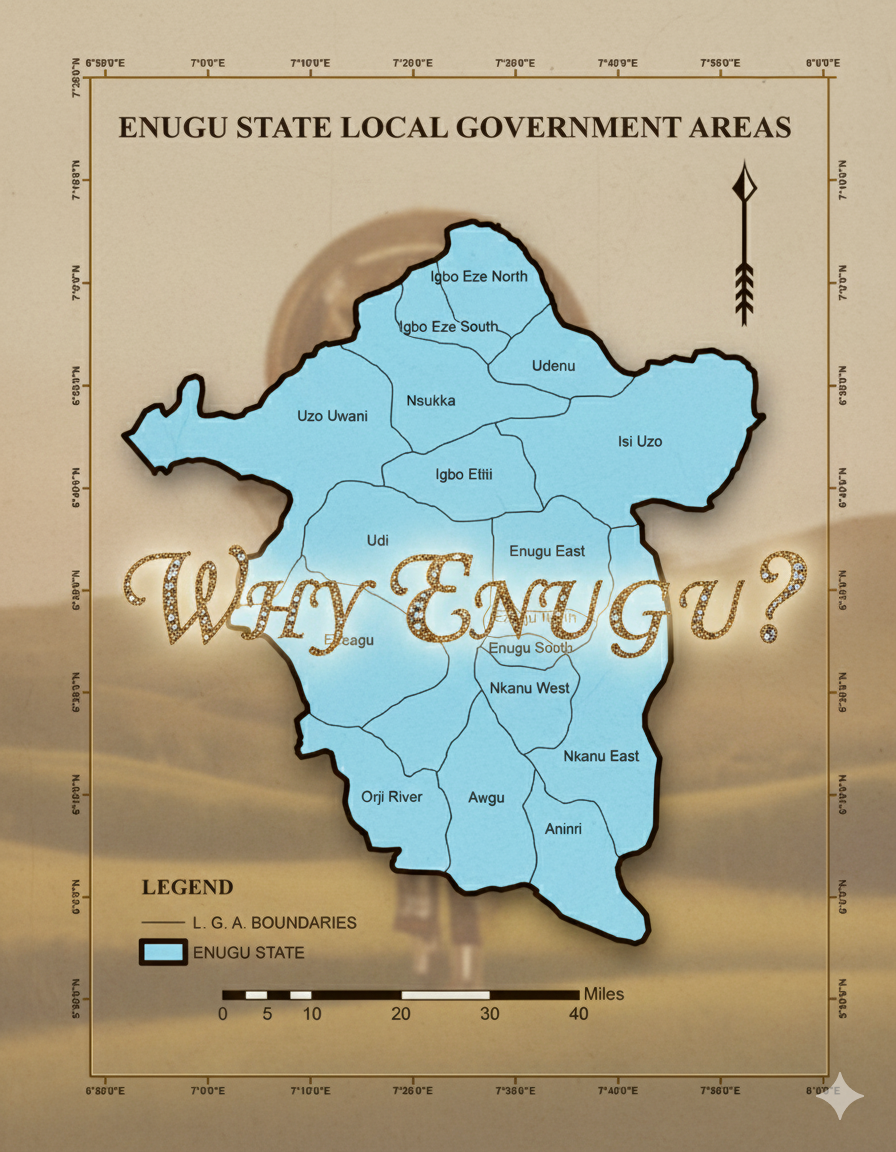
Enugu State, South-East Nigeria
Enugu carries a specific tradition in medical history: its scientists and institutions have repeatedly produced solutions designed not for ideal conditions, but for the real-world constraints of resource-limited settings. From community-directed disease control to non-invasive diagnostics and preventive pharmaceutical innovation, the recurring logic has been anticipation over reaction. The Institute of Preemptology formalises that trajectory.
A State-Wide Infrastructure in Formation — Enugu is constructing a network of 260 modern Primary Healthcare Centres, one in every political ward of the state. This expanding infrastructure offers the IoP an immediate community-level platform for preventive care from the first day of operations.
A Powerhouse of Medical Education — Enugu is home to accredited institutions including the University of Nigeria Teaching Hospital and leading medical universities. This established academic base allows the IoP to draw on existing talent, infrastructure, and a culture already oriented towards clinical excellence.
A Documented Record of Medical Foresight — Enugu's scientific contributions share a common quality: they were designed to intercept disease.
Enugu's expanding PHC network is being unified through a comprehensive Electronic Health Record system, providing the IoP a real-time data platform for tracking and validating preemptive interventions with precision.
Enugu has a long-standing tradition of inclusivity — embracing diversity across ethnicity, social background, and belief. These values reflect the Institute's own commitment to equitable, community-centred health. A founding institution requires a broad foundation, and Enugu provides one.
The IoP Complex is a medical institution built from first principles, in the place where the conditions are hardest and the need is greatest. Those who support it now take part in its founding — in the creation of an institution that will outlast them.
Copyright © 2025 The Institute of Preemptology (a mass medical mission project). All rights reserved.